Auto Billing
Reliable Auto-billing is the headache-less future.
In an industry that balances on this feature, it should be the most rock solid. Imagine automatic: Modifiers per insurance; Incident-too per insurance; Deductible Accounting; Auto-eligibility checks when possible; Secondary Claims.
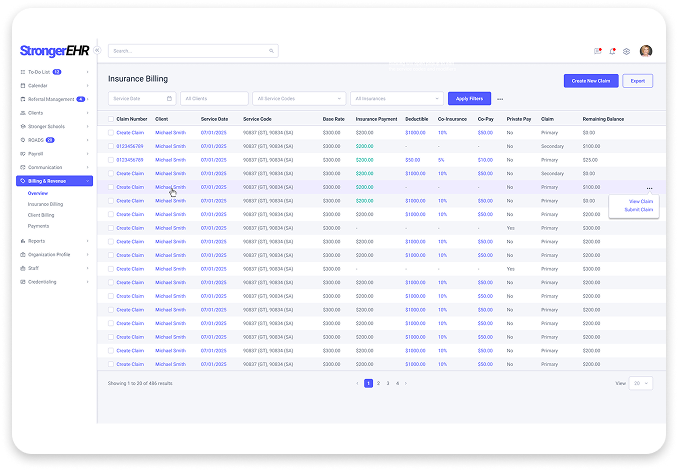
Your Billing Specialists will be trouble-shooters instead full-stop doers.
The arrival of StrongerEHR will be game-changing for your billers. A milestone akin to going from by-hand to drive-thru car washes except this system picks it up once it is completely made. No driving necessary.
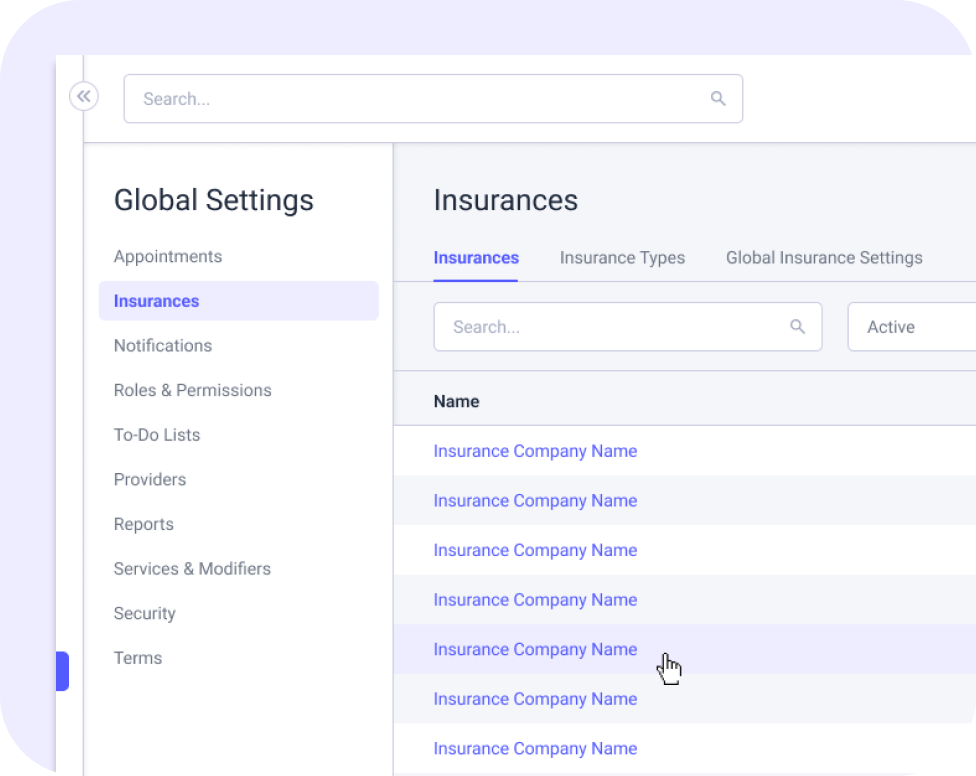
Insurance Modifiers
Simply set up the rules in our EHR and rely upon the auto entry into every applicable claim. Multiple variables can be taken into consideration such as: location; provider type; insurance and more.

Eligibility Checks
Although not impermeable, we have sought the best apparatus to automate eligibility on a monthly basis at a low cost. Decrease the likelihood of denials with automation that even asks the client’s for monthly updates as a double measure. Maybe don’t tell your biller about this if you don’t want them to pressure you on your software decision.

Incident-too Billing
Whether it is because a provider is out or you have associate-level providers, it is a manual burden to facilitate this your-self. We have automated it. Your Biller is now free to do something else.
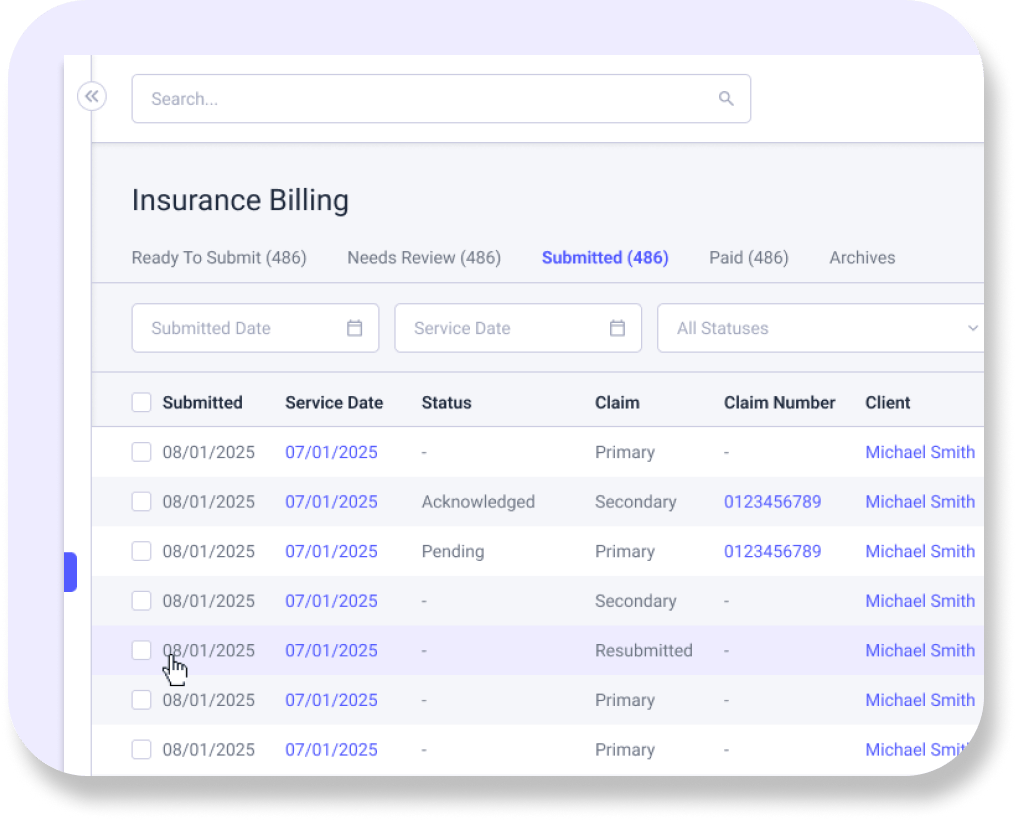
Secondary Claims
The bane of most Biller’s existence can be automatically submitted, correctly, the first time. Ask how your Biller feels about such a feature.

Deductible Accounting
The bridge of a client’s benefits changing is hard to plan for with so many to manage. We track all payments to estimate this change so that it can be proactively navigated and updated when multiple providers are being utilized.
Intake that works like you do—automated, intuitive, and easy to engage.
- Individuals can freely find services & fill out one application for all of them.
- Organizations can freely find Individuals in need and receive direct referrals/leads.
- Easily manage referrals/leads via the ToDo Task Manager. Outside tasks welcomed!
- Easily stay connected with calendar & tele-health video conferencing! *
- Interoptibility Future
- Internal communication that is Secure/HIPAA compliant.
- Secure document creation and storage. Make your resume or letter here!
Relationship management, communication, and compliance all in one place.
- All the features of StrongerACCESS plus...
- Built in AI Assistant
- Automated Medical Billing with all the complexities worked out. Save time and money.
- Human Resources project flows with training & reminders so that nothing is missed.
- Accounting with Automation & Payroll Integration
- Multistate support
- Integrated Teams-Based-Care
Smart tasking, AI-powered notes, streamlined billing, and full credentialing—all tailored to the way you provide care.
- All the features of StrongerCRM plus....
- Integrated Measured-Based-Care for grant outcomes, quality measures and contractual requirements.
- Customizable Insurance Rules to audit proof your organization from monetary take backs.
- Integrated state level reports (ROADS) for easing administrative burdens.
- Semi-Automated Credentialing for easy tracking.
- All the tools to prescribe
- Integrated Multi- State Reporting
- Built in AI Note Taker

Feature Eyebrow TEXT
Yorem ipsum dolor amet, consecte adipiscing elit.
Porem ipsum dolor sit amet, consectetur adipiscing elit. Nunc vulputate libero et velit interdum, ac aliquet odio mattis.
Call to action title text here in this spot.
Yorem ipsum dolor sit amet, consectetur adipiscing elit. Nunc vulputate libero et velit interdum, ac aliquet odio mattis.